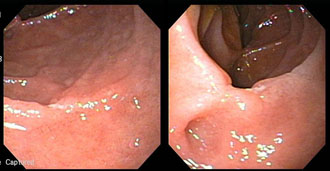
Crohn’s disease is an ongoing (chronic) disorder that causes inflammation of the digestive or gastrointestinal (GI) tract from the mouth to the anus. The most common area is in the end of the small intestines (the ileum) and/or the beginning of the large intestine (the colon). The swelling there extends deep into the lining of the affected organ causing pain and diarrhea. (see picture below).
Crohn’s disease and Ulcerative Colitis are two diseases that belong in a larger group called Inflammatory Bowel Disease (IBD). Both are related to an abnormal response by the body’s immune system. Researchers believe the body’s immune system sends white blood cells to attack the bacteria naturally found in the intestines. This causes inflammation. These white cells then make harmful products which lead to ulcerations and bowel injury. The result is IBD. (see picture below).
Studies show inflammation in IBD is caused by several factors: it runs in families (genetics), the immune system, and something in the environment. Antigens in the environment may be the direct cause of inflammation because they stimulate the body’s immune system to respond with inflammation that continues out of control and doesn’t shut off. Crohn’s disease patients have immune systems that attack the intestines and sometimes the eyes, skin, or liver. It is not known why this occurs.
It is estimated that as many as 1.4 million Americans have IBD. Crohn’s affects approximately 10% of children younger than 18 years old. IBD is most often found affecting whites—especially those with Eastern European Jewish descent—but increasingly is reported in African Americans. Rates for Hispanics and Asians are lower than both whites and African Americans.
Symptoms
Symptoms of Crohn’s disease can range from mild to severe and may develop gradually or come on suddenly. There may be times when there are no symptoms. When active, symptoms may include:
- Persistent diarrhea, sometimes with blood and mucus
- Abdominal pain and cramping
- Blood in the stool
- Ulcers
- Reduced appetite and weight loss
- Unexplained fevers and tiredness
- Eye inflammation
- Mouth sores
- Skin disorders
- Arthritis
- Fever
- Inflammation of the liver or bile ducts
- Delayed growth or sexual development in children.
Complications
Crohn’s may lead to several complications which include:
- Bowel obstruction. Parts of the bowel can thicken and narrow which blocks the flow of digestive contents passing through the affected part of the intestine. Surgery may be necessary to remove the affected portion of the bowel.
- Ulcers. Chronic inflammation can lead to open sores (ulcers) in any area of the digestive system from mouth to anus.
- Fistulas. Ulcers can extend completely through the intestinal wall creating a fistula.
- Anal fissure. This is a crack, or cleft, in the anus or in the skin around the anus where infections can occur.
- Malnutrition. Diarrhea, abdominal pain and cramping may make it difficult to eat or for the intestine to absorb enough nutrients. Anemia is common in people with Crohn’s.
- Colon cancer. Having Crohn’s that affects the colon increases the risk of colon cancer.
- Other health problems such as:
- Arthritis
- Inflammation of the eyes or skin
- Clubbing of the fingernails
- Kidney stones
- Gallstones
- Inflammation of the bile ducts
- Osteoporosis (weak, brittle bones).
Diagnostic Tests
The doctor may suspect Crohn’s disease based on the patient’s medical history, but testing is needed to know for sure. Various diagnostic tests are available to help confirm a diagnosis:
- Blood tests – to check for anemia or signs of infection.
- Fecal occult blood test – tests your stool for blood.
- Prometheus® IBD7 Serology Test – genetic blood test used to determine IBD.
- Colonoscopy– the entire colon can be viewed using a thin, flexible, lighted tube with an attached camera.
- EGD – a fiberoptic endoscope, with a camera, is place down the throat to the stomach and duodenum. A tissue sample can be taken for a biopsy.
- Computerized tomography (CT) – a special X-ray that looks at the entire bowel and tissues outside the bowel that can’t be seen with other tests.
- Magnetic resonance imaging (MRI) – uses a magnetic field and radio waves to create detailed images of organs and tissues.
- Capsule endoscopy – a capsule is swallowed that has a camera inside. The camera takes pictures and sends them to a computer that is worn on a belt. Once it goes through the digestive system, the camera leaves your body in the stool.
- Small Bowel Follow Through –looks at the part of the small bowel that can’t be seen by a colonoscopy. After drinking a solution, an X-ray, CT or MRI images are taken of the small intestines.
Treatment
The goal in treating Crohn’s disease is to reduce the inflammation causing damage to the intestines. While there is no cure for Crohn’s, several treatments have proven to be effective in controlling symptoms. Some of the medications the doctor may prescribe are: (for more detail see the medications section):
- Aminosalicylates (5-ASA) – anti-inflammatory drugs like Asacol, Colazal, Dipentum, Pentasa, Azulfidine, and rectually Canasa or Rowasa
- Corticosteroids – suppress the immune system and used to treat moderate to severely active Crohn’s – Prednisone and budesonide
- Antibiotics – metronidazole and ciprofloxacin
- Biologic therapies – Remicade, Humira, Cimzia
- Immuno-modulators – Purinethol, Imuran, methotrexate
- Nutritional liquid formulas
Sometimes a patient is admitted to the hospital as part of the treatment plan. Hospitalization may occur for a few days or a few weeks. During this time, it is common for the doctor to place the patient on total parenteral nutrition (TPN) to allow the bowel to rest. The patient will not eat or drink anything during this time. Later, clear liquids will be allowed. The patient can go back to eating regular foods when the doctor approves.
Dietary changes may also be helpful to maintain optimal nutrition. Consider meeting with one of our dietitians for a nutritional consult. Call (865) 546-3998 to schedule an appointment.
Additional Resources
Living with Crohn’s Disease: www.livingwithcrohnsdisease.com
Crohn’s and Colitis Foundation of America: www.ccfa.org
Remicade: www.remicade.com
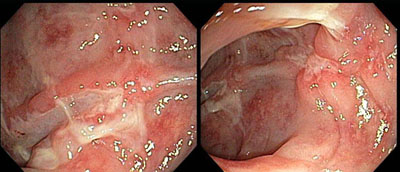
Deep Linear Ulcerations in Crohn’s
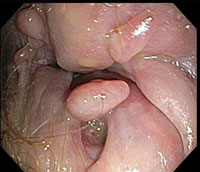
Perirectal Fissure and Fistula
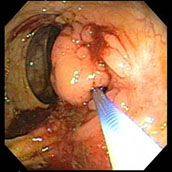
Fistula
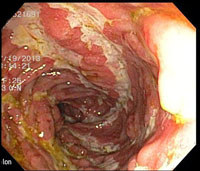
Crohn’s: in acending colon